These are the results of an anonymous questionnaire regarding mental health in the gastroparesis community. The survey was open for a one-week period from September 25 to October 1, 2019, and was posted publicly on Facebook and Twitter as well as in our closed Gastroparesis Support Group (and several subgroups) and in our Gastroparesis: Fighting for Change advocacy groups. We had 784 total respondents.
Please note that this survey is intended only to inform and should not be interpreted as scientifically proven data or as implying any sort of causation between mental and physical health. Those of us conducting the survey are not researchers, and though we do our best to present and interpret findings, we seek primarily to spark interest in further research among those properly qualified to conduct it. In addition, as a community, we wish to know more about our fellow community members, and these surveys give us an indication of the circumstances and difficulties others face. In assessing the results, we find numerous limitations and shortcomings associated with this questionnaire, but we learn as we go and hope to conduct follow-up surveys to better enlighten us about the conditions in which this community finds itself.
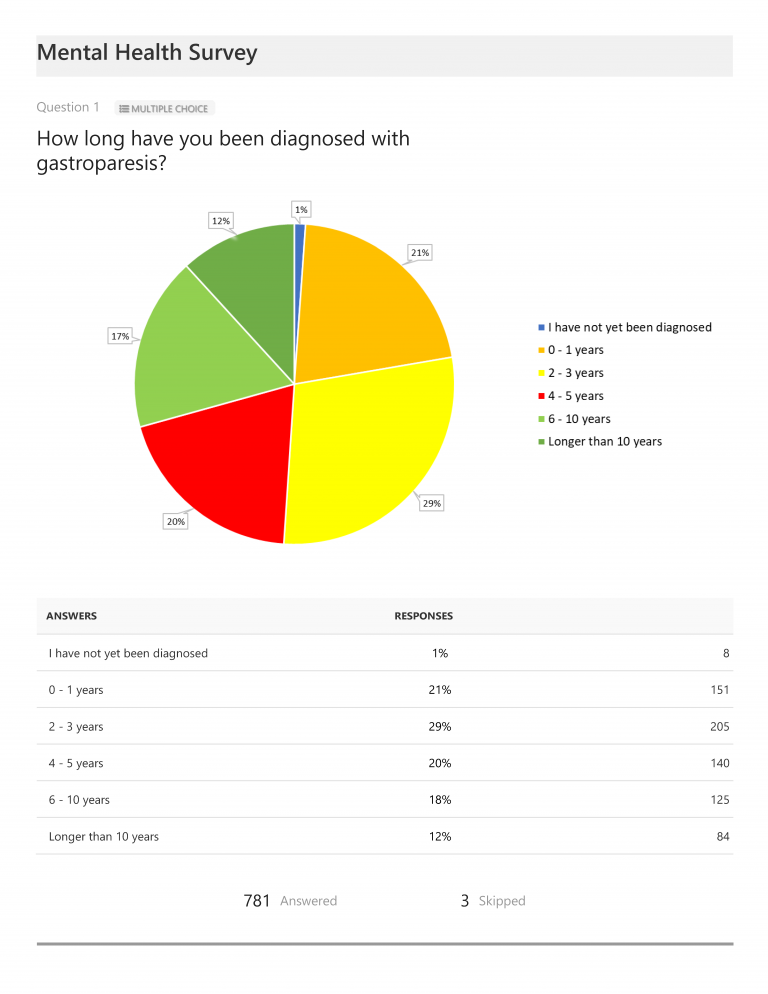
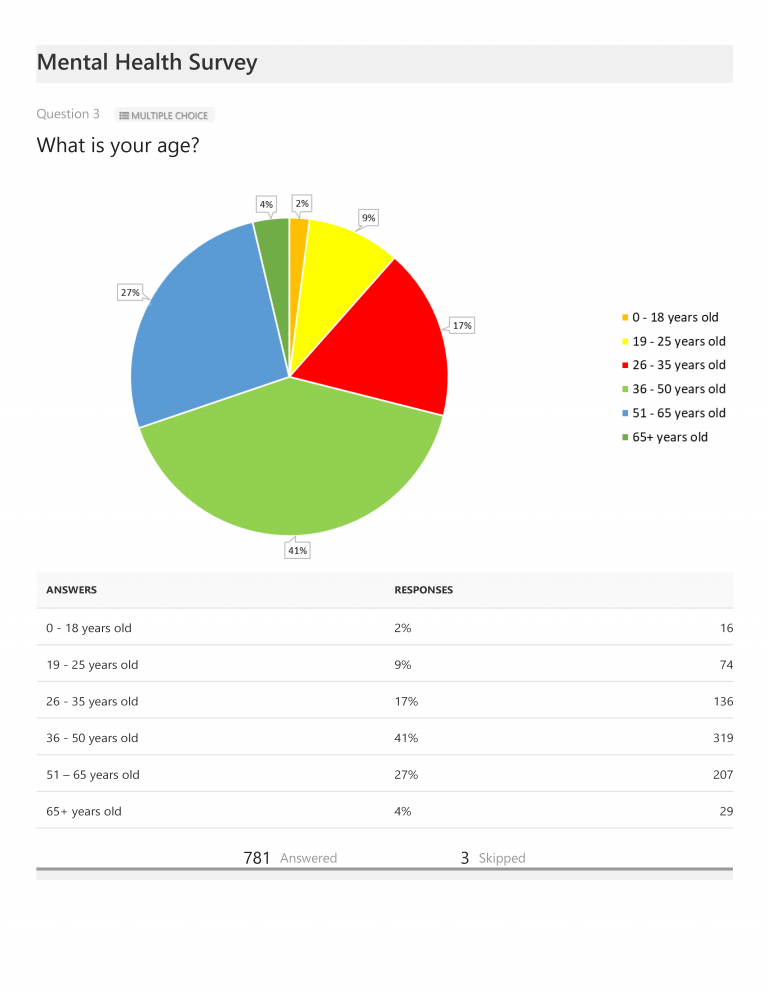
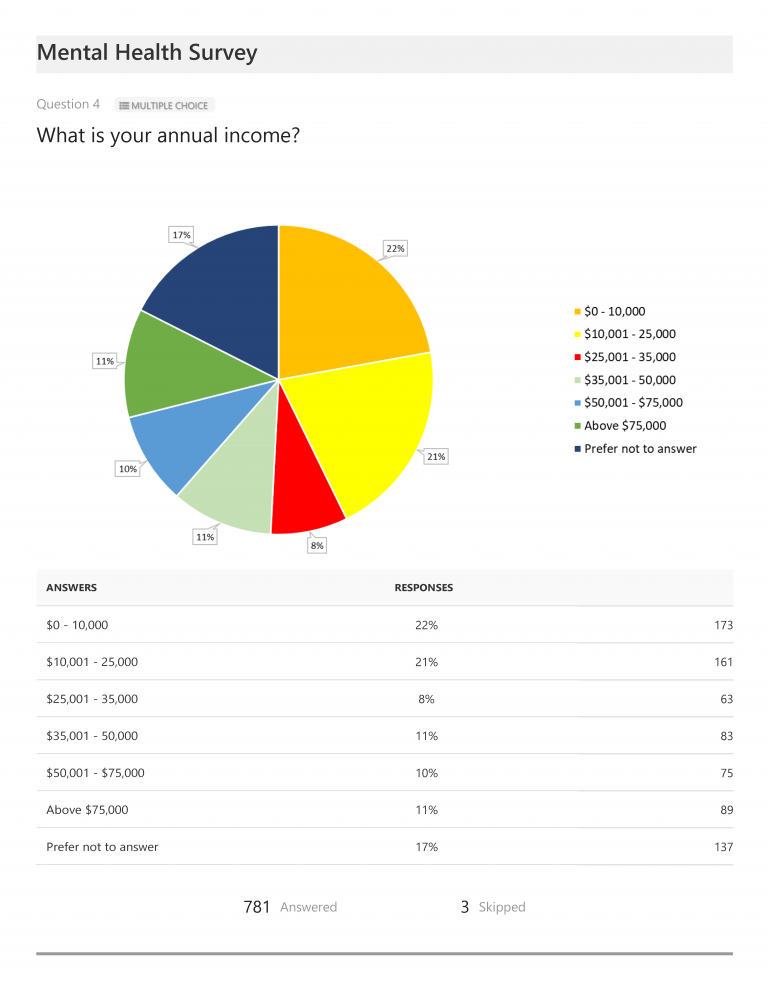
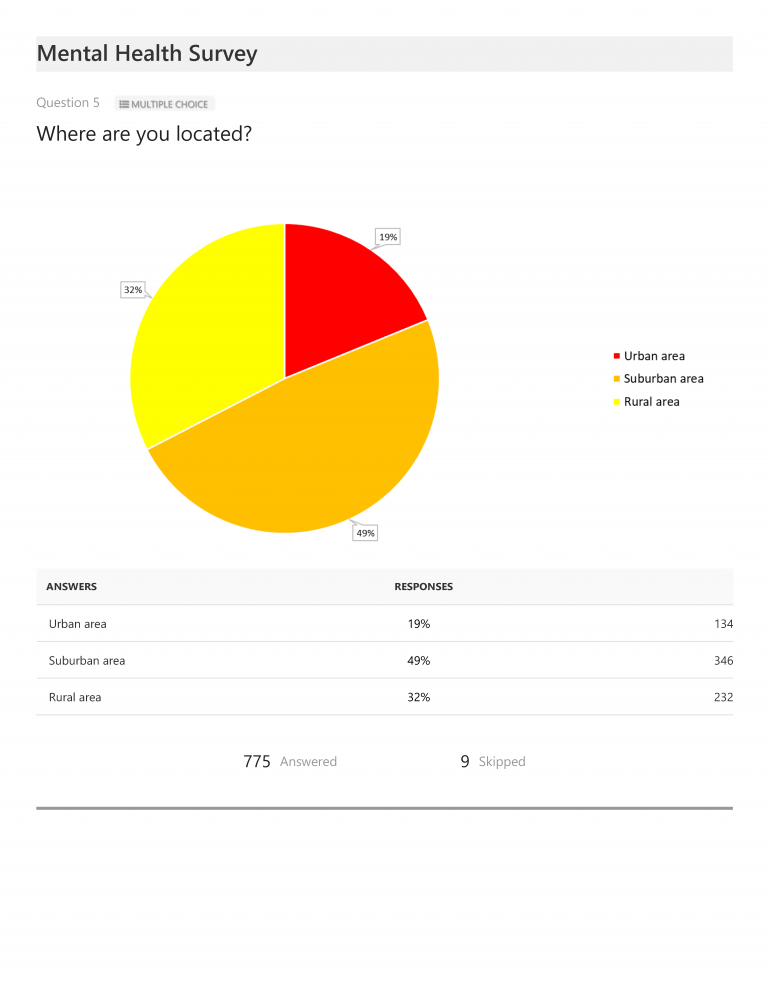
Regarding the results, the first few charts show participants’ gender, age, annual income, general location, and number of years since being diagnosed. Of those completing the survey, 95% of respondents (or 744) identified as female, and 41% fell into the 36-50 year old category. 67% had been diagnosed between 2-10 years, 21% for less than one year, and only 12% had been diagnosed more than 10 years ago. Annual income varied greatly, with only 11% earning above $75,000 per year and 22% noting income of $10,000 per year or less. 68% indicated they reside in either urban or suburban areas (49% suburban; 19% urban) and 32% in rural areas.
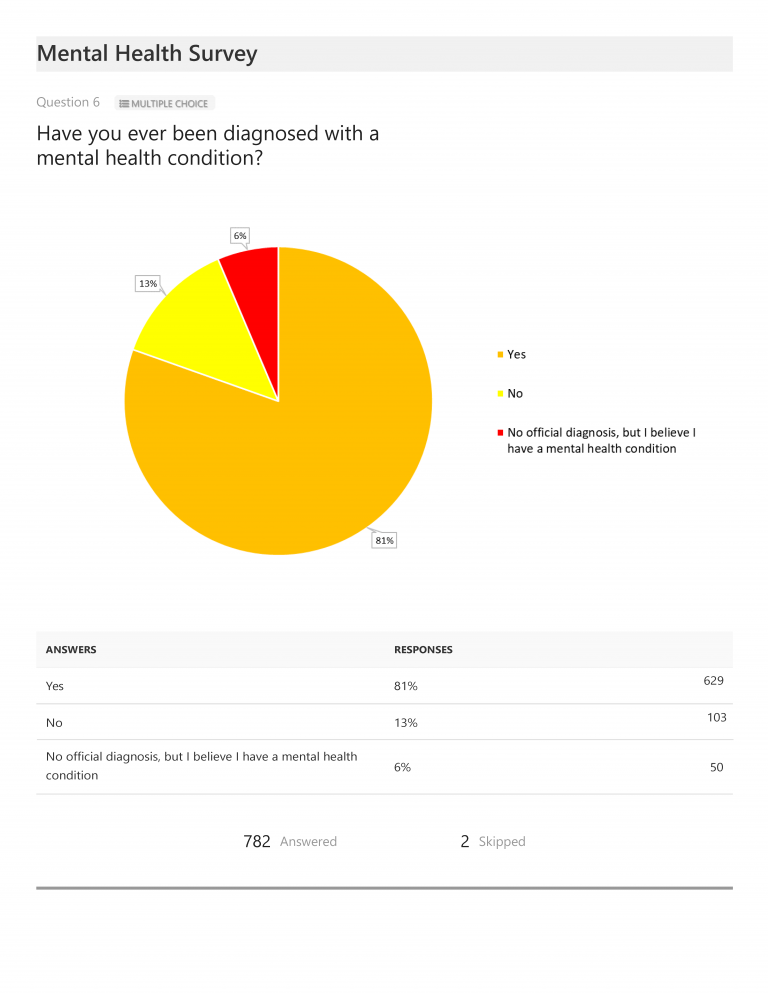
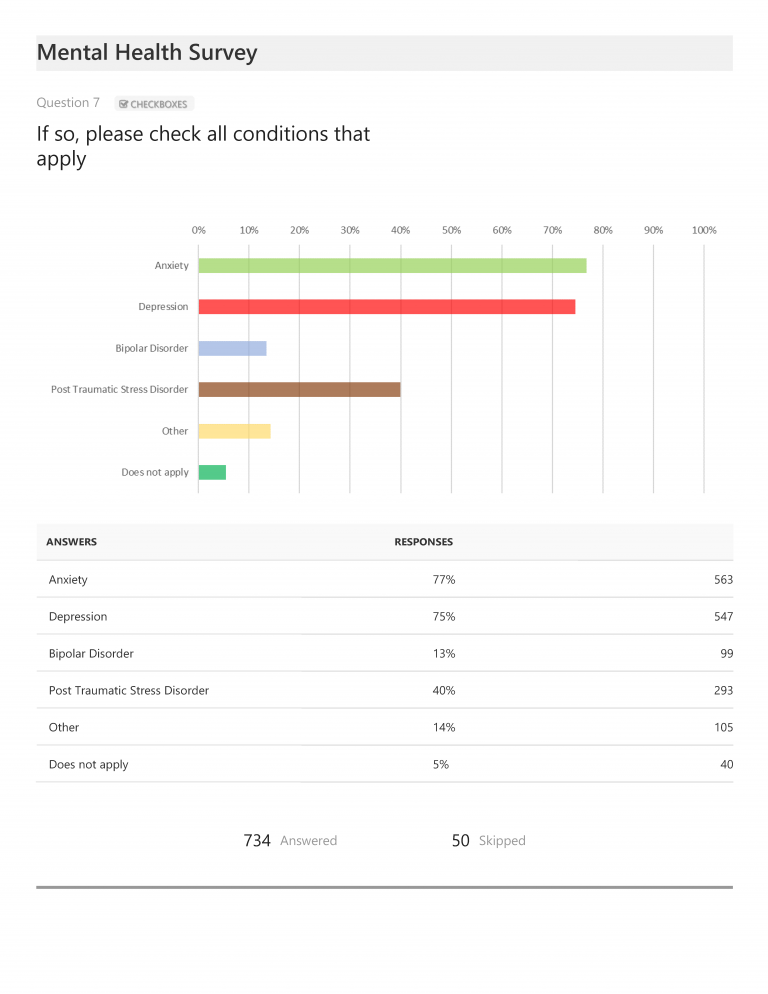
When asked if they had ever been diagnosed with a mental health condition, 81% (or 629) responded that they had and another 6% (or 50) responded that, while they had not been given an official diagnosis, they believe they live with a mental health condition. When asked about their specific mental health diagnoses (and permitted multiple responses), anxiety (77%) and depression (75%) were most commonly cited, followed by PTSD (40%). Additional mental health conditions not included in the response options (but listed as “other” in written questionnaire responses) included eating disorders, borderline personality disorders, obsessive-compulsive disorders, ADHD, panic attacks/disorders, and several others. [It is worth noting that, while not included in our chart presentation, 524 respondents (or approximately 67% of total respondents) cited more than one mental health diagnosis. The most commonly cited combination was anxiety and depression, with 59% of total respondents (or 464) noting they had been diagnosed with both.]
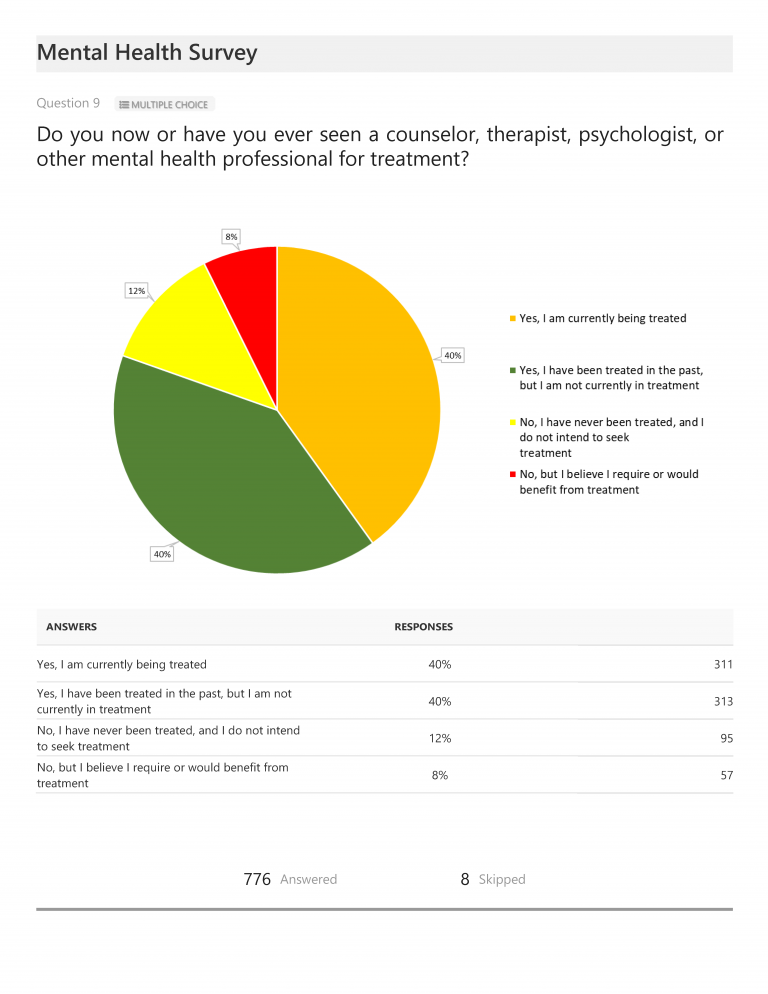
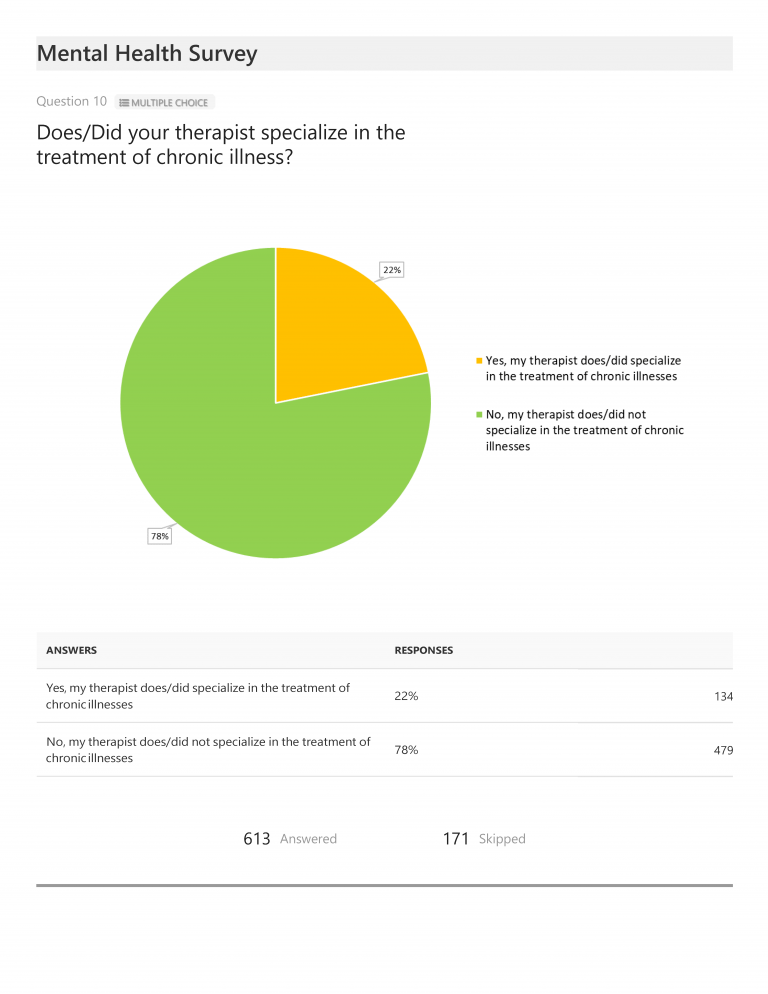
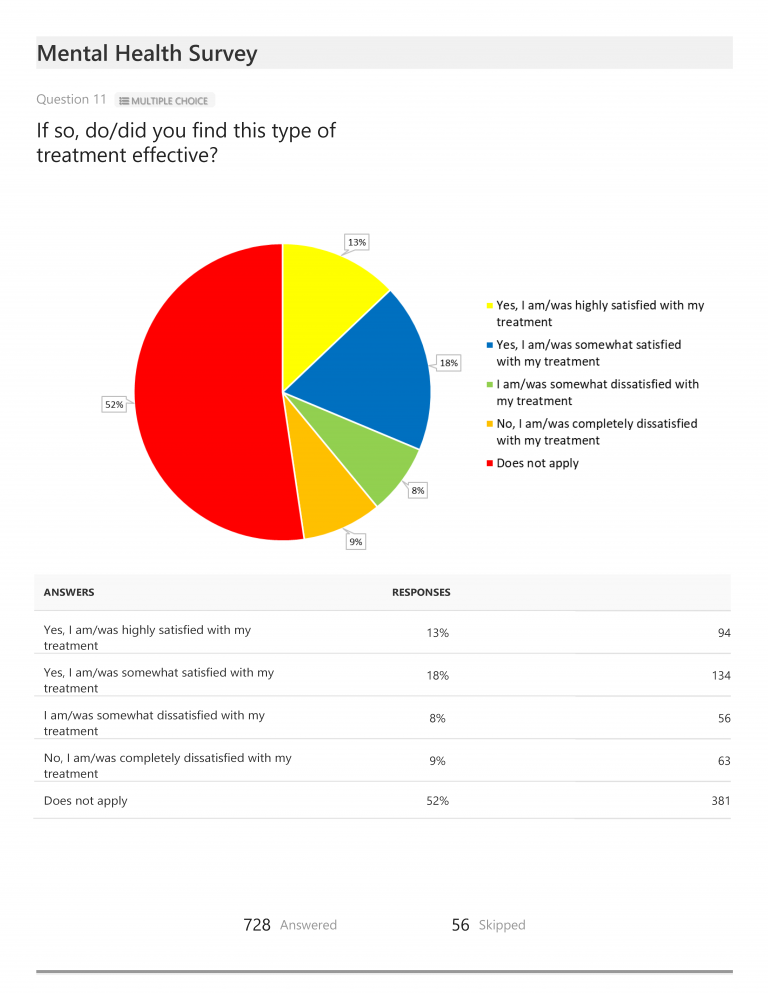
Approximately 80% of total respondents indicated they either were currently being treated for a mental health condition (40%) or that they had been treated in the past (40%). Another 8% responded that they had never been treated but believed they would benefit from treatment. When asked if they found treatment to be effective, 31% replied that they found treatment to be either highly (13%) or somewhat (18%) effective and 17% replied that they were either somewhat or completely dissatisfied with their treatment. (For reasons we cannot fully understand, 52% selected “Does not apply” when asked this question.) Of those who were currently receiving or had previously received treatment, only 22% indicated their therapist specialized in the treatment of chronic illnesses. [While not included in our chart presentation, of the respondents receiving treatment from a therapist specializing in chronic illness, 90% noted that they were either highly (49%) or somewhat (41%) satisfied with their treatment.]
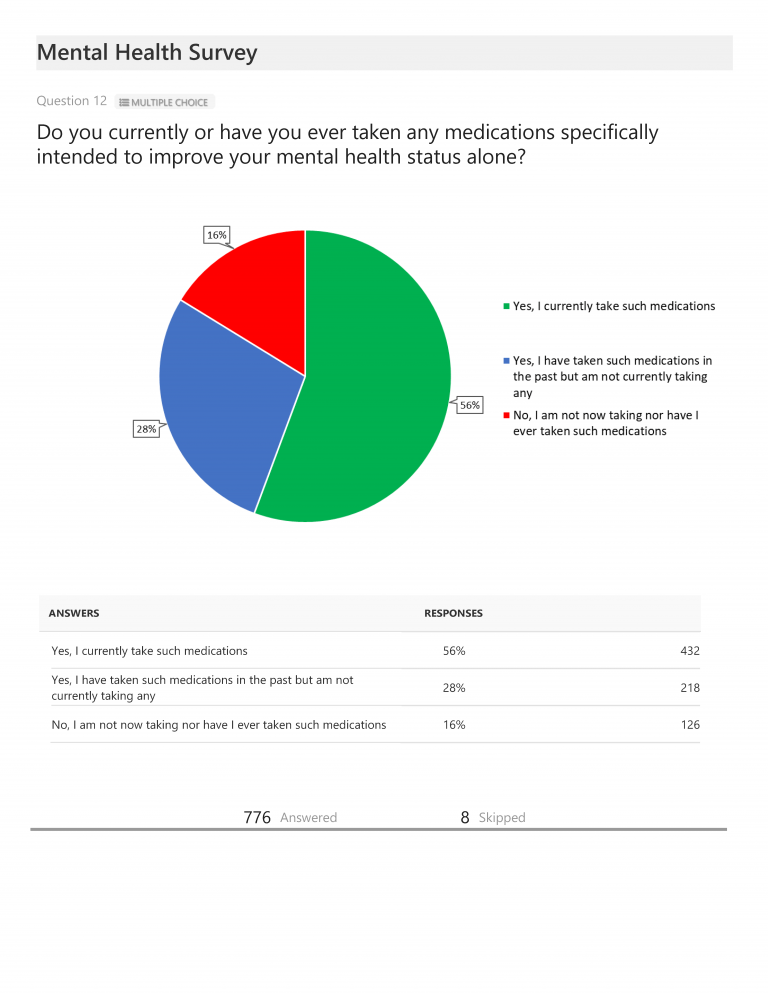
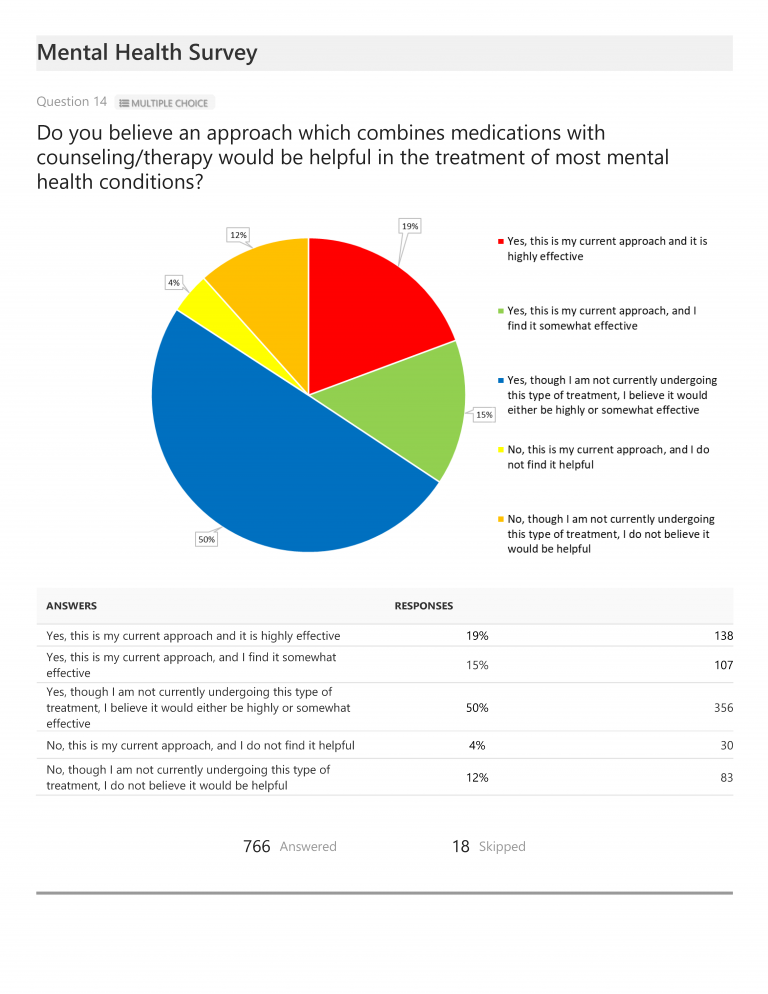
When asked about medications, 84% of total respondents indicated they were either currently taking medications specifically intended to improve their mental health status (56%) or that they had taken them in the past (28%) and 68% noted that these medications were either highly (23%) or somewhat (45%) effective. When asked if they believed an approach which combined medications(s) with counseling would be helpful for most mental health conditions, 50% responded that, though they were not currently undergoing this type of treatment, they believed it would be helpful. Another 34% indicated that this was either their current treatment approach or a previous approach and that it was highly (19%) or somewhat (15%) effective.
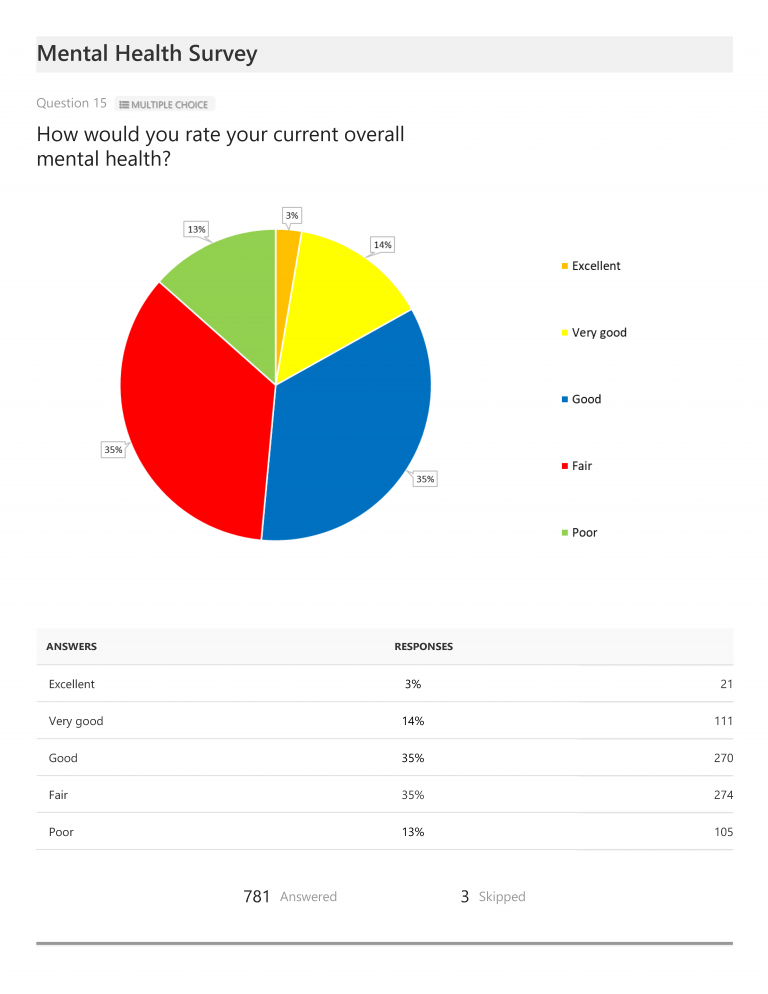
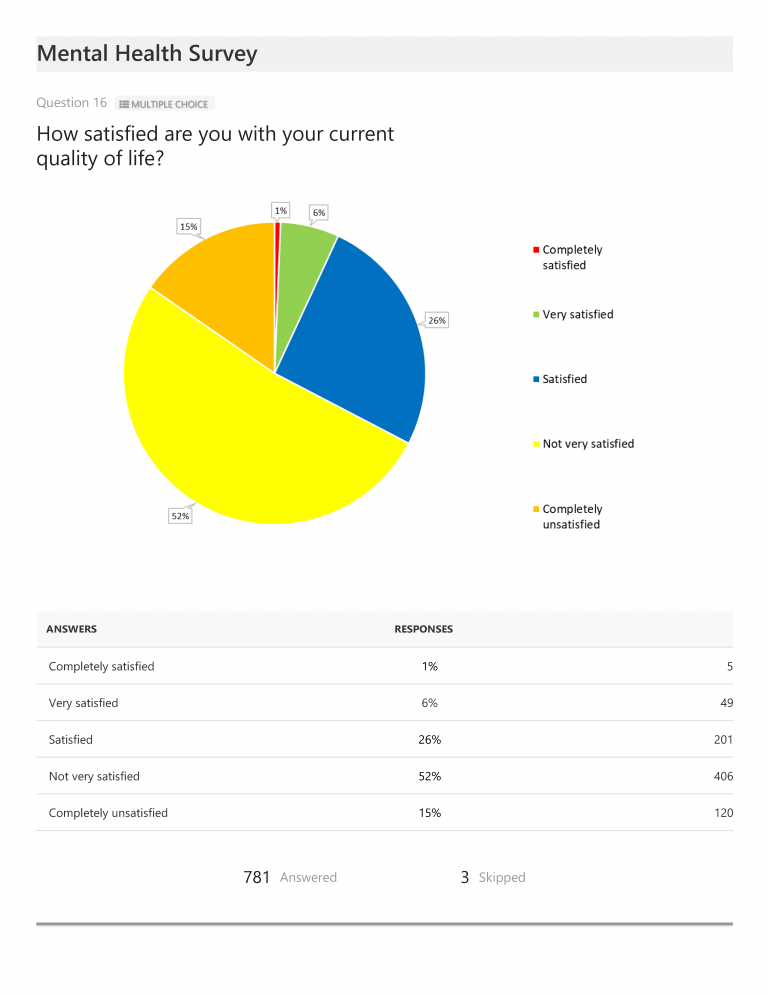
In terms of current overall mental health, as self-assessed, 35% of total respondents rated their mental health as good, 17% rated it very good or excellent, and 48% rated it fair or poor. When asked to self-assess quality of life, 67% responded that they were either not very satisfied (52%) or completely unsatisfied (15%), 26% were satisfied, and only 7% were either very (6%) or completely (1%) satisfied. Of the 784 total respondents, 628 (or 80%) who had been diagnosed with a mental health condition echoed these numbers, with 69% indicating they were either not very satisfied (53%) or completely unsatisfied (16%) with their quality of life. (The quality of life ratings did not vary greatly from these figures regardless of the number of years respondents had been diagnosed: 67% of those diagnosed for 1 year or less were either not very satisfied or completely unsatisfied; 2-3 years = 67%; 4-5 years = 66%; 6-10 years = 64%, and 10 years or longer = 73% either not very satisfied or completely unsatisfied with their quality of life.)
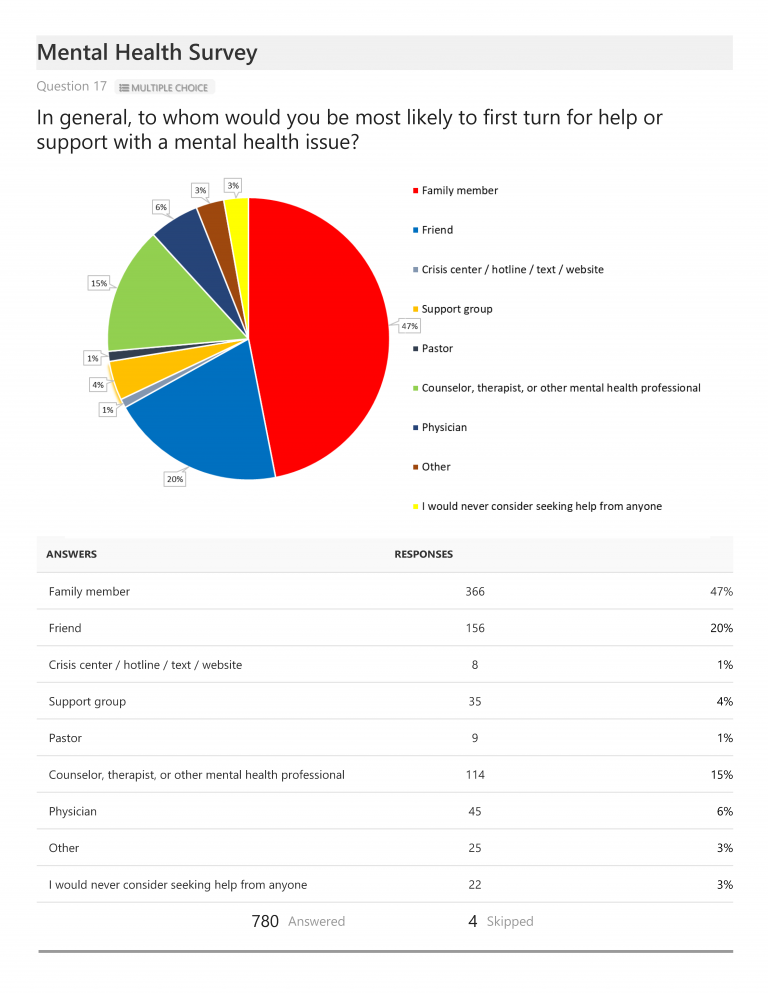
When asked to whom they would first turn for help with a mental health condition, 67% responded that they would seek support from either a family member (47%) or friend (20%) and 15% indicated they would first seek help from a mental health professional. Only 1% responded that they would first seek help from a crisis center or hotline.
Several respondents also submitted comments with their questionnaire, and we have included a sampling of those below.
As noted above, there are many limitations and shortcomings associated with this survey. First and foremost, we wish we had asked respondents the estimated date of their mental health diagnoses. It would have been interesting to note whether the physical diagnosis preceded the mental health diagnoses or vice versa. We also wish some of the questions had been a bit clearer. For instance, the question regarding income was designed to gauge household income, but because we failed to specify, we are not certain whether responses indicate individual or household income. In addition, because our survey largely targets Facebook, we cannot assess those outside of social media. Facebook limits accounts to those above 13 years of age as well, so we have very few if any respondents in that age category.
We would love to make further assessments as well. We wonder whether and how age, location, and income have any bearing on the type and quality of treatment patients receive and on whether they have adequate access to this care. We wonder what factors patients consider when evaluating the effectiveness of treatment, their overall mental health rating, and quality of life measures. We would also like to know why patients value certain sources above others for help and support and whether that varies depending on the seriousness of the mental health condition or in the event of a true crisis. We wish we better understood the connection between physical and mental health, if one exists, and would like to know details about the impact of one upon the other as experienced by patients, in their own words. And, finally, we would love to hear from patients as to what most needs to change in terms of how mental health is addressed and how we might go about implementing solutions to the problems this community faces.
We intend to pursue follow-up surveys, but our real hope lies in garnering the support of those scientists and physicians who might take an interest in this too-often-neglected gastroparesis community and reach out to us for further in-depth study regarding these matters. We are grateful to all who participated and to all who take the time to review the survey results.
Thank you!